The Omicron variant is considered to potentially hold the key to helping humanity overcome Covid-19, especially as vaccines have not led to herd immunity.
Currently, data collected from various countries show that Covid-19 vaccines, or even natural infections, do not provide a permanent immune defense against the risk of SARS-CoV-2 virus infection. This reality means that the goal of achieving herd immunity is becoming increasingly elusive.
However, with the emergence of the Omicron variant, scientists believe that the virus will help a large portion of the global population develop “super immunity” – meaning better resilience against new variants or even any future coronavirus strains.
Super immunity does not eliminate the risk of virus infection entirely, but it may help infected individuals experience only mild symptoms or remain asymptomatic, allowing life to return to normal, according to the Wall Street Journal.
Benefits of Contracting Covid-19
To understand why Omicron signals the potential end of the pandemic, it is important to highlight the benefits that vaccination or natural Covid-19 infection brings to individuals.
In the human body, there are two types of white blood cells: T cells and B cells. These white blood cells are responsible for identifying and eliminating invading pathogens.
T cells act like patrol soldiers, circulating through the bloodstream and lymph nodes. When they detect a foreign virus, T cells become activated.
One type of T cell, known as cytotoxic T cells, destroys cells that have been invaded by pathogens. Another type, helper T cells, sends signals to B cells, activating the production and release of antibodies that neutralize the pathogens.
Typically, after the virus and infected cells have been eliminated, the army of white blood cells and antibodies also dissipates. However, some white blood cells can remember the virus long-term and enhance their resistance; these are known as memory T cells.

People waiting for Covid-19 testing in New York. (Photo: New Yorker).
Memory T cells reside in the bone marrow, lymph nodes, and other tissues. If a pathogen invades again, memory T cells will quickly activate the entire immune system to attack and eliminate the pathogen.
Meanwhile, memory B cells concentrate in lymph nodes. The first infection helps these cells remember and subsequently produce antibodies capable of blocking new variants. When the virus returns, B cells can produce antibodies more quickly and effectively.
Vaccines simulate the infection phenomenon, training the immune system by introducing weakened viruses or antigens into the body. For Covid-19, pharmaceutical companies use the spike protein – the part that allows the virus to attach to human cells.
Antibodies produced after vaccination tend to diminish faster than those from natural infection, possibly because actual virus components remain in the body longer than antigens.
Vaccination or natural infection helps train the immune system to respond more robustly, quickly, and accurately to subsequent infections.
Omicron as the Key
Research indicates that the immune system of individuals who have been infected with the SARS-CoV-2 virus and then vaccinated will produce more antibodies and retain them longer than those who are only vaccinated.
A study by the Oregon Health & Science University published in December 2021 found that vaccinated individuals who later contracted Covid-19 had antibody levels up to 1,000 times higher than those who received only two vaccine doses.
Scientists note that contracting Covid-19 before or after vaccination will create “super immunity.”
“Super immunity does not mean we will end Covid-19, but it provides a path out of the pandemic. If vaccinated individuals later contract the virus, they will be significantly protected against other virus variants in the future,” said Dr. Marcel Curlin, a researcher at Oregon Health & Science University.
A study from South Africa showed that individuals infected with the Omicron variant produced antibodies that neutralized the Delta variant with four times greater efficacy.
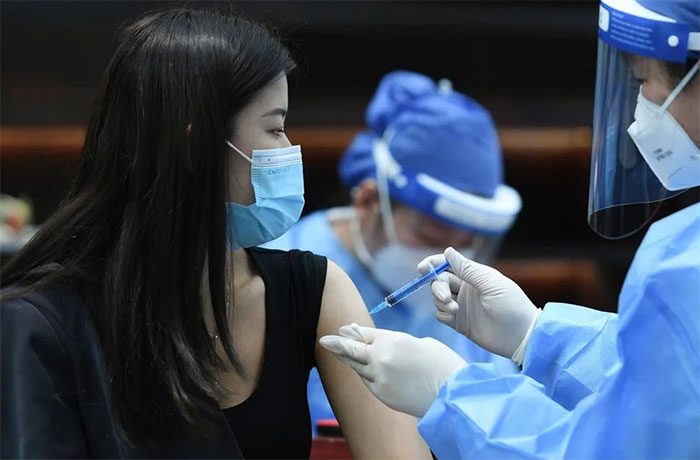
Covid-19 vaccination in China. (Photo: SCMP).
A booster shot also enhances the immune response by extending the time B cells learn about pathogens. This result explains why antibodies produced after three doses of the Pfizer vaccine can effectively neutralize the Omicron variant, while only two doses do not.
However, the booster shot only trains the immune system to recognize the same target, which is the spike protein. The numerous mutations on the Omicron variant require immune cells to work harder, thereby strengthening the immune response.
T cells in vaccinated individuals can respond effectively to the Omicron variant at a rate of 70-80%, reducing the risk of severe illness or death from Covid-19.
Natural infection further enhances T cell capabilities, enabling them to recognize other viral proteins, not just the spike protein. Some of these proteins share characteristics with proteins found in the SARS virus or common cold-causing coronaviruses.
Additionally, T cells from individuals who contracted SARS 17 years ago can recognize parts of the current SARS-CoV-2 virus. A study from Imperial College London showed that individuals who had previously contracted a cold caused by a coronavirus had a lower risk of contracting Covid-19.
Data suggests that infection with the Omicron variant is likely to stimulate the production of an effective and long-lasting immune response against Covid-19, even against other coronavirus strains, even if they mutate and become more virulent.
As the Omicron variant continues to spread, individuals who have been vaccinated or previously contracted Covid-19 have the opportunity to develop “super immunity” if they continue to be reinfected. As a result, Covid-19 could eventually become a virus that causes a common illness like the flu, which is uncomfortable but rarely fatal.