Early identification of emergency signs in cardiovascular diseases and appropriate initial management can help patients avoid unfortunate outcomes later on.
Below are several emergency situations related to cardiovascular issues:
1. Cardiac Arrest
Signs of Cardiac Arrest: The patient suddenly collapses, loses consciousness, does not respond when spoken to, exhibits total body cyanosis, shows no signs of breathing, and there is no detectable carotid or femoral pulse. Involuntary urination or defecation may occur.
In this situation, it is crucial to quickly provide first aid to the patient while calling for assistance from those nearby and asking someone to call emergency services at 115 immediately. Quickly place the patient on a hard surface and begin chest compressions and rescue breaths.
The proper technique for chest compressions is as follows: The rescuer kneels beside the victim, places their right hand over the left hand, and positions both hands on the lower third of the sternum. Apply firm pressure with both hands to compress the chest. You need to perform continuous compressions, even without rescue breaths if you are alone. If assistance is available, you can alternate compressions, continuing until medical personnel arrive or the patient regains consciousness.
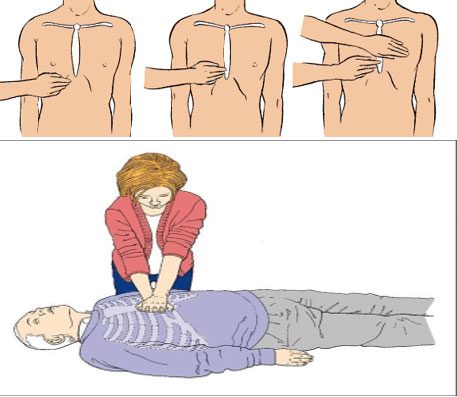
External chest compression.
2. Chest Pain During Myocardial Infarction
After exertion (heavy work, exercise, sports, walking, climbing stairs, etc.), the patient may suddenly experience severe pain in the left chest or behind the sternum, feeling as if being squeezed in the chest or crushed, with pain radiating to the jaw, left shoulder, inner left arm, or to the back. Cold sweats may accompany the pain… The pain may last for about 5-10 minutes or longer. This is a suspected symptom of chest pain in myocardial infarction.
When encountering a patient with these symptoms, it is vital to quickly have them sit comfortably, reclining slightly, loosening any belts or ties, and simultaneously call for emergency services at 115. Try to calm the patient, encouraging them to breathe deeply and slowly, which can help alleviate chest pain and reduce anxiety. If you cannot call an ambulance, ask those nearby for help in transporting the patient to the nearest hospital, avoiding allowing the patient to drive themselves.
3. Acute Stroke
The signs of an acute stroke are abbreviated as F.A.S.T, which includes: F (Face): sudden facial asymmetry, drooping mouth; A (Arm): numbness or weakness on one side (arm and leg on the same side); S (Speech): slurred speech or inability to speak; T (Time): take the patient to the nearest medical facility with a stroke center because the “golden time” for the brain lasts only about 4.5 to 6 hours, and can extend to 9 hours from the onset of symptoms.

Signs of acute stroke abbreviated as F.A.S.T.
If the patient receives emergency treatment within this timeframe, the chances of recovery are very high. Many cases may suddenly become sluggish, respond poorly to questions, or exhibit visual disturbances (sudden blindness, blurred vision, double vision…), or experience severe headaches accompanied by nausea…
When encountering patients exhibiting these symptoms, avoid the following actions:
- Do not allow the patient to eat or drink anything.
- Do not self-administer brain supplements or stroke medications.
- Do not perform blood tests on the fingertips.
- Do not delay resting further to wait for these symptoms to subside.
It is essential to quickly: record or photograph any medications the patient is currently taking, note the onset time of symptoms, and promptly transport them to the nearest hospital with a stroke center. This information will greatly assist the medical team in treating the patient, reduce waiting time, and provide significant benefits for the patient. If the patient loses consciousness, has no breathing or heartbeat, proceed with resuscitation for cardiac arrest.
4. Shortness of Breath
The patient suddenly experiences difficulty inhaling or exhaling, rapid breathing, and may speak in short phrases while sweating profusely. Position the patient with their head elevated (using one or two pillows) or sitting on a chair, leaning slightly forward or against a wall. A comfortable sitting position will help the patient relax and stabilize their breathing; loosen clothing, belts, or ties, provide oxygen if available, or use a hand fan to circulate air over their face and nose. Then, promptly call emergency services at 115 or ask for help to take the patient to the nearest hospital.
Community first aid and initial emergency response should be provided as quickly as possible to maintain the patient’s vital functions in the best condition before reaching the hospital. Therefore, developing an external emergency response system and equipping individuals with basic first aid knowledge will help reduce the risk of death and minimize injuries for patients in critical situations, especially beneficial for families with elderly members, young children, or relatives with cardiovascular diseases or underlying health conditions that require monitoring.