It is hard to find a symbol more fitting for the current Covid-19 pandemic than the N95 respirator mask. This mask fits snugly around the face and can filter up to 95% of tiny particles in the air, such as viruses and toxic smoke, something that other equipment (like surgical masks) cannot achieve. This life-saving gear is now in short supply globally and represents the most extreme challenges the world is facing in the fight against Covid-19.
The Birth of the N95 Mask
So how did such a fragile polymer cover become the most important medical device of the 21st century – especially in the current context? It all began in 1910 with a little-known doctor who wanted to rid the world of one of the worst diseases ever known.
The First Mask Designs
According to Christos Lynteris, a senior lecturer at the School of Social Anthropology at the University of St. Andrews, long before we knew that bacteria and viruses could spread through the air and cause illness, people were using face masks – but not necessarily to prevent the spread of disease.

Plague doctor mask from the 17th century.
At that time, people believed that diseases like the plague were caused by miasma, or toxic air rising from the ground. This belief led to the design of famous plague masks throughout Europe in the 1600s. These elongated masks resembled bird beaks and had two breathing holes on the sides where incense (or herbs) could be placed.
People thought that by preventing themselves from smelling the miasma of the plague, they would not be infected with the deadly disease. Doctors – tasked with identifying outbreaks – would wear these masks and mark infected individuals by tapping their canes.
It wasn’t until the 1870s that scientists learned more about bacteria, and the miasma theory was gradually debunked along with the horrific design of the plague mask.

A depiction of the eerie appearance of historical plague doctors.
From 1897, doctors began to wear surgical masks while working. However, at that time, they were no different from a handkerchief wrapped around the face, and they were not designed to filter airborne pathogens – even now they are not. They were simply meant to prevent the doctor from coughing or sneezing into the wound during surgery.
This is the most significant difference between masks and respirators. This is also why healthcare professionals were very concerned when they were advised to wear surgical masks while interacting with Covid-19 patients, without respirators. These respirators are made from a different type of material than surgical masks and fit tightly to the face, allowing for maximum air filtration.
The First Respirator – Born from Plague and Stigma
In the fall of 1910, an outbreak occurred in Manchuria – at that time a complex contested area between Russia and China. While this disease caused a terrifyingly high mortality rate, up to “100% of infected individuals, no one survived” – as Lynteris noted – it also sparked a scientific race. Both Russia and China wanted to demonstrate their scientific capabilities to assert their claims of sovereignty.
The Chinese side sent a young doctor named Wu Lien-Teh to lead their efforts. Although he graduated from Cambridge, among the large team of international scientists and doctors from around the world studying this deadly disease, Wu became “completely insignificant.” However, after examining a corpse, Wu concluded that the disease spread through the air, not through fleas as many suspected.

Healthcare workers wearing masks during the pneumonia outbreak in Manchuria in 1910.
With this conclusion and based on the surgical masks he had seen in the West, Wu designed a sturdier mask made from gauze and cotton, which could wrap tightly around the face and was supplemented with multiple layers of fabric to filter the air. His invention was a breakthrough at the time, but it was met with skepticism and derision from his colleagues.
Lynteris stated: “There was a famous old doctor in the area, a French doctor (Gérald Mesny) … and when Wu explained to the French doctor his hypothesis that this disease was pneumonia and spread through the air, the Frenchman insulted him … in a stigmatizing way, saying “What can we expect from a Chinese person?” To prove his point, Mesny went in and treated patients in the hospital without wearing Wu’s mask, and he died two days later from the disease.“
Even though other doctors in the area quickly developed their own versions of masks, Wu’s mask triumphed over all. It had an excellent design. It could be handmade from inexpensive and readily available materials.
From January to February of 1911, the production of masks skyrocketed as everyone wore them. From healthcare workers to soldiers, some even wore them daily. Not only did these masks help prevent the spread of the disease, but they also became a symbol of modern medicine.
By the time the Spanish flu emerged in 1918, Wu’s mask became even more famous in both scientific circles and the public. Companies worldwide ramped up production of similar masks to help mitigate the spread of the flu.

Transport staff and passengers wearing masks during the 1918 flu pandemic.
And Then the N95 Mask Was Born
The N95 mask is a descendant of Wu’s design. During World War I and II, scientists invented gas masks that enclosed the user’s head to purify inhaled air. Similar masks, but with added fiberglass filters, began to be used in the mining industry to prevent black lung disease.
Although effective in protecting health, they were quite bulky and heavy. The main reason lay in the filters. Additionally, fiberglass made breathing more difficult, and the head-enclosing design caused the wearer to overheat. Therefore, this posed a danger to those working in construction environments, as they often inhaled asbestos but did not want to wear these masks due to the already hot construction sites.

Type of gas mask used in World War I.
Thus, by the 1970s, the Mine Safety and Health Administration established the first criteria for “disposable respirators.”
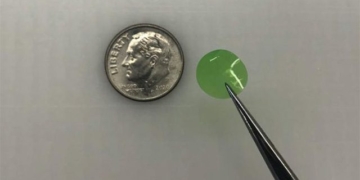
The company 3M was the first to develop the disposable N95 dust mask, which was approved in 1972. Instead of using fiberglass, the company repurposed a technology they had previously developed for creating stiffer filter strips. They used melt-blown polymer and blew it into fine fiber layers to make these fibers stiffer and used them as filters.
As a result, particles in the air, whether silica dust or viruses, would be trapped in the maze of these stiff fibers as they passed through the filter. Additionally, 3M added an electrical charge to this filter material, helping to attract even smaller particles to these fibers. Meanwhile, because the gaps between these fibers were relatively large, users could still breathe easily.
However, at some point, when these gaps become filled with these fine particles, breathing will become more difficult. That is why the N95 mask cannot be used for more than 8 hours at a time in dusty environments. It still filters smoke and particles afterward, but breathing becomes more challenging, which is why it needs to be replaced daily.
Decades later, the N95 mask gradually found its way into various industries before the demand for respirators surged in the 1990s due to the resurgence of drug-resistant tuberculosis.

The N95 mask is designed to fit snugly to the user’s face, including children.
To prevent the spread of tuberculosis bacteria in the air, the N95 mask became standard equipment for healthcare workers, and doctors began wearing them to assist tuberculosis patients. Even so, these respirators are rarely used in hospitals today, with demand only spiking during outbreaks like the current Covid-19 pandemic.
In China, respirators like Wu’s design have always been crucial for the country. Most recently, during the SARS outbreak, the Chinese population had to wear these face protections to prevent the disease’s spread. Later, as cities like Beijing faced air pollution, people also increased their use of masks to filter toxic air.
The N95 mask is not perfect. It is designed to fit snugly against the user’s face, including children and those with facial hair, but if not sealed properly, it will not perform as advertised. Furthermore, variants of the N95 intended for high-risk environments do not have exhalation valves, which can make the wearer feel hot when worn.
However, the N95 mask has undergone hundreds of years of development to tackle various crises. This development will continue even after the Covid-19 pandemic subsides. 3M has stated that the company is continuously reassessing the N95 mask, refining its components from the filter to its ergonomic shape.
Nikki McCullough, head of the Occupational Safety and Health Department at 3M, stated: “… we want them to look simple so they are intuitive and easy to use. We are always improving the technology. We have thousands of scientists at 3M researching it.“